- Chronic disease management dominates healthcare budgets, putting unsustainable cost pressure on care systems.
- Workforce shortages and burnout are undermining care delivery.
- Fragmented, reactive care models are failing to meet rising demand.
Our Advice
Critical Insight
- Healthcare leaders face unclear reimbursement and policy frameworks, with inconsistent billing codes, funding models, and regulatory uncertainty slowing enterprise adoption.
- Clinicians struggle with data integration and overload, as interoperability gaps and fragmented IT systems leave providers overwhelmed by alerts and paperwork instead of patient care.
- Patient trust, engagement, and access remain inconsistent, with concerns about data privacy, low digital literacy in older populations, and connectivity issues in rural and underserved regions.
- Scaling remote patient monitoring (RPM) is no longer optional, chronic disease costs, workforce shortages, and fragmented care models demand urgent change. CIOs must confront reimbursement gaps, solve interoperability issues, and embed RPM into enterprise virtual care strategies to unlock sustainable value.
Impact and Result
- Review emerging RPM trends and frameworks to understand their impact on people, processes, technology, and data.
- Evaluate organizational readiness to support RPM trends by analyzing maturity across people, processes, technology, and data. Assess interoperability, workflow alignment, workforce capacity, and governance practices to understand the current state.
- Set the course for enterprise adoption by prioritizing the most critical gap-closure initiatives, aligning them with strategic objectives, and building a clear implementation roadmap.
Scale Remote Patient Monitoring to Improve Healthcare Services
Shifting RPM from projects to organizational strategy.
Analyst perspective
Integrate and scale your RPM programs to optimize costs and efficiency.

The rising cost of chronic disease management, workforce shortages, and fragmented, reactive care models are placing unsustainable pressure on healthcare systems. Most organizations have begun adopting remote patient monitoring (RPM), but too often programs remain siloed pilots that fail to deliver enterprise-wide impact.
Healthcare leaders must move beyond incremental implementations to scaling RPM as a strategic capability. Scaling enables organizations to address reimbursement gaps, align fragmented workflows, and integrate with enterprise data governance, unlocking sustainable financial and operational benefits.
The real opportunity lies not in launching more isolated RPM initiatives, but in building an integrated RPM ecosystem that spans people, processes, technology, and data. By embedding RPM within digital health strategy, organizations can reduce the long-term technology costs of managing fragmented programs, increase patient engagement, and create a scalable model for managing high-cost chronic care populations.
This research equips CIOs and executives with a roadmap to evaluate readiness, close capability gaps, and scale RPM adoption. Scaling RPM doesn’t just contain costs – it positions healthcare organizations for long-term resilience by transforming chronic care management into a sustainable, data-driven enterprise function.
Sharon Auma-Ebanyat
Research Director, Healthcare Industry
Info-Tech Research Group
Executive summary
Your Challenge |
Common Obstacles |
Info-Tech’s Approach |
|---|---|---|
|
|
|
Info-Tech Insight
Scaling remote patient monitoring is no longer optional; chronic disease costs, workforce shortages, and fragmented care models demand urgent change. CIOs must confront reimbursement gaps, solve interoperability issues, and embed RPM into enterprise virtual care strategies to unlock sustainable value.
Identify emerging RPM trends transforming care models: From projects to strategy
RPM is moving from pilots to enterprise scale with AI, wearables, virtual wards, and equitable access defining the next era of proactive, patient-centered care.
01 AI-Driven Predictive & Proactive Monitoring
RPM is increasingly empowered by artificial intelligence (AI) and predictive analytics, enabling early detection of patient deterioration and triggering alerts for timely intervention.
02 Next-Gen Wearables & Sensor Integration
Wearables have evolved from fitness trackers to medical-grade, multi-sensor devices capable of monitoring ECG, glucose, oxygen levels, and more with a growing focus on interoperability standards
03 Hospital-at-Home/Virtual Wards Expansion
The “hospital-at-home" model, or virtual wards, is trending upward, delivering high-acuity care in patients’ homes through telemonitoring, wearable sensors, and remote oversight. These models offer potential cost savings and reduced readmissions.
04 Equitable RPM Access in Rural/ Underserved Areas
RPM paired with telehealth is pivotal for extending healthcare to rural and underserved communities, especially where physical access to clinics is limited.
Confront rising costs and workforce strain in healthcare
Healthcare cannot sustain rising chronic disease costs and workforce burnout with fragmented delivery; scaling RPM is no longer optional, it’s essential for system survival.
Chronic Disease Burden
- Chronic non-communicable diseases (diabetes, cardiovascular, respiratory, etc.) continue to dominate healthcare costs worldwide.
- These conditions now account for the majority of healthcare spending and are projected to keep rising as populations age and care demand intensifies.
- Traditional episodic care delivery is insufficient to meet the ongoing needs of this growing patient population.
Workforce Shortages & Burnout
- Healthcare systems face severe staffing crises that limit their ability to scale chronic care programs.
- Physician shortfalls and nurse burnout are accelerating, with large percentages of the workforce considering leaving the profession.
- Workforce strain threatens access, quality, and continuity of care.
Fragmented Care Delivery (Silos & Admin Burden)
- Most RPM deployments remain siloed, limited to pilots or disease-specific programs without enterprise-wide integration.
- Clinicians lose valuable time navigating disjointed systems, undermining efficiency and patient experience.
- Without seamless interoperability, the full promise of proactive monitoring is not realized.
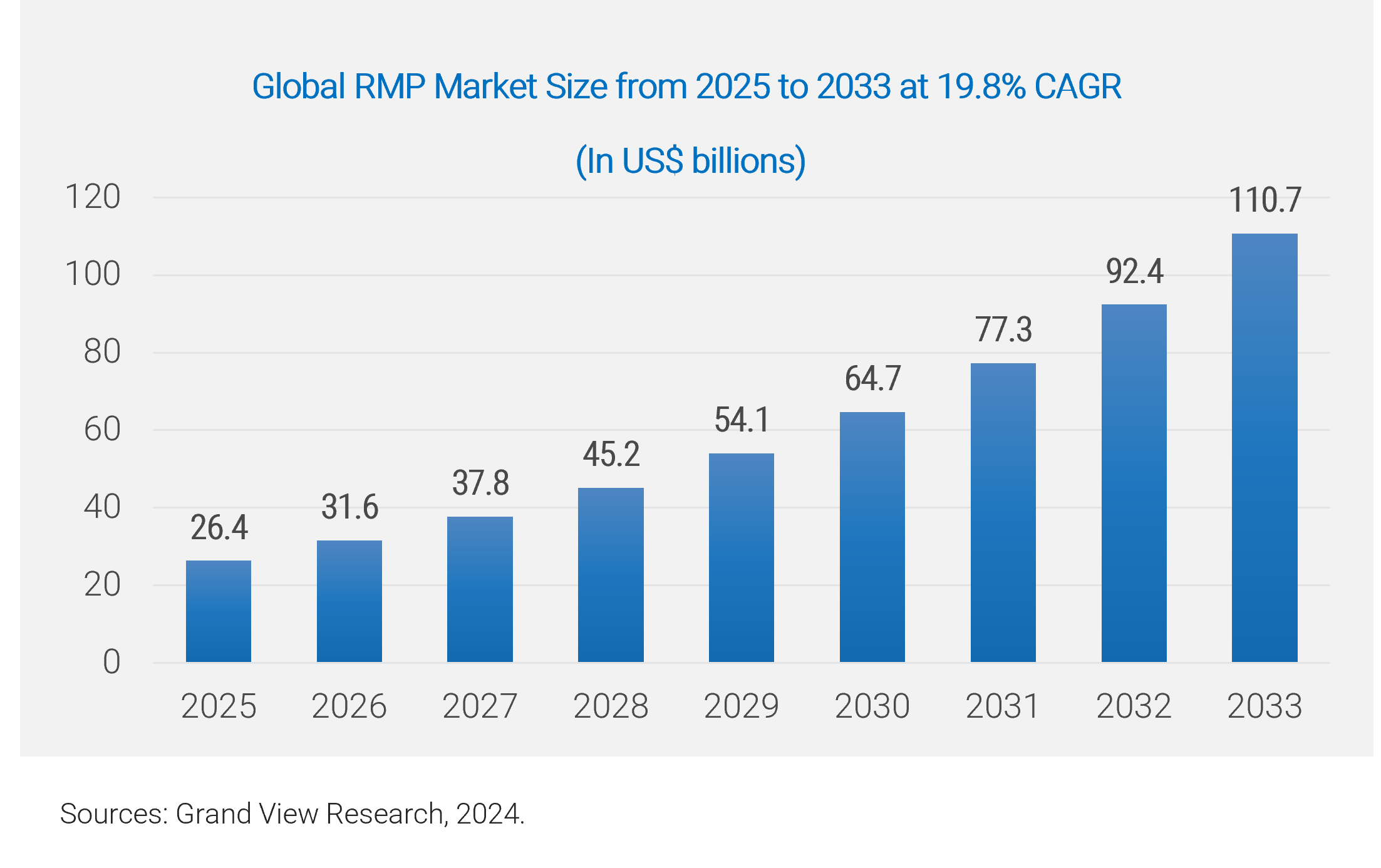
The remote patient monitoring market is growing
Remote patient monitoring is expanding rapidly, signaling a critical shift in care delivery.
Factors impacting growth
Chronic disease costs: Rising rates of diabetes, heart failure, and COPD drive RPM adoption to cut readmissions and long-term care expenses
Tech integration & AI: Wearables, predictive AI, and EHR interoperability make RPM more accurate, scalable, and enterprise-ready.
Workforce shortages: RPM automates monitoring and triage, extending care teams and addressing staff burnout.
Equity & reimbursement: Expanded Medicare/commercial coverage and rural broadband programs enable RPM access for underserved populations.
Overcome key obstacles to scaling RPM effectively
Scaling RPM requires overcoming policy, data integration, and patient engagement hurdles.
- Unclear reimbursement and policy frameworks
Healthcare leaders face unclear reimbursement and policy frameworks, with inconsistent billing codes, funding models, and regulatory uncertainty slowing enterprise adoption. - Data integration challenges increase clinical workload
Clinicians struggle with data integration and overload, as interoperability gaps and fragmented IT systems leave providers overwhelmed by alerts and paperwork instead of patient care. - Patient engagement and literacy challenges
Patient trust, engagement, and access remain inconsistent, with concerns about data privacy, low digital literacy in older populations, and connectivity issues in rural and underserved regions.
Transform IT into a strategic enabler of RPM
RPM turns IT into a strategic driver by enabling data-driven care, automation, and stronger interoperability.
Challenges |
⟩ | Common Obstacles |
⟩ | Opportunities |
|---|---|---|---|---|
Chronic Disease Burden Workforce Shortages & Burnout Fragmented Care Delivery (Silos & Admin Burden) |
|
Data-Driven Population Health Management Virtual Care Infrastructure Expansion Workforce Optimization Through Automation Strengthened Interoperability & Security Leadership |
Embed RPM into your digital health strategy
A digital health strategy aligns IT and business priorities into a single organizational roadmap that drives care quality, workforce efficiency, and financial sustainability.
Strategic Alignment
- Chronic disease costs drive >90% of US healthcare spend; RPM delivers early detection and proactive management, directly advancing business goals of cost containment and quality (CDC, 2025).
- CIOs who embed RPM into the digital roadmap move it from “pilot projects” to a pillar of enterprise virtual care delivery.
Technology & Integration
- By integrating RPM into the EHR (orders, notes, alerts), you avoid “swivel-chairing” between systems and enable clinical workflows.
- Aligning with national interoperability frameworks (e.g. TEFCA) helps ensure your RPM vendor strategy supports data liquidity and scaling.
Workforce & Operations
- With projected clinician shortages, RPM enables team-based models (nurses, physician assistants) to extend capacity and reduce burnout.
- Embedding RPM from the start ensures workload models, escalation paths, and clinical workflows are built explicitly for distributed care.
Financial & Patient Impact
- Hospital-at-Home programs show lower post-discharge spending and positive patient outcomes relative to inpatient care.
- Positioning RPM within digital strategy strengthens investment cases: fewer readmissions, lower resource use, better ROI.
Info-Tech Insight
Embedding RPM into the digital health strategy unifies IT and business strategy, enabling scalable care models, sustainable operations, and measurable patient impact.
Identify your organization’s business and IT capabilities for scaling RPM
Business capability map defined…
In business architecture, the primary view of an organization is known as a business capability map.
A business capability defines what a business does to enable value creation, rather than how. Business capabilities:
- Represent stable business functions.
- Are unique and independent of each other.
- Typically will have a defined business outcome.
A business capability map provides details that help the business architecture practitioner direct attention to a specific area of the business for further assessment.
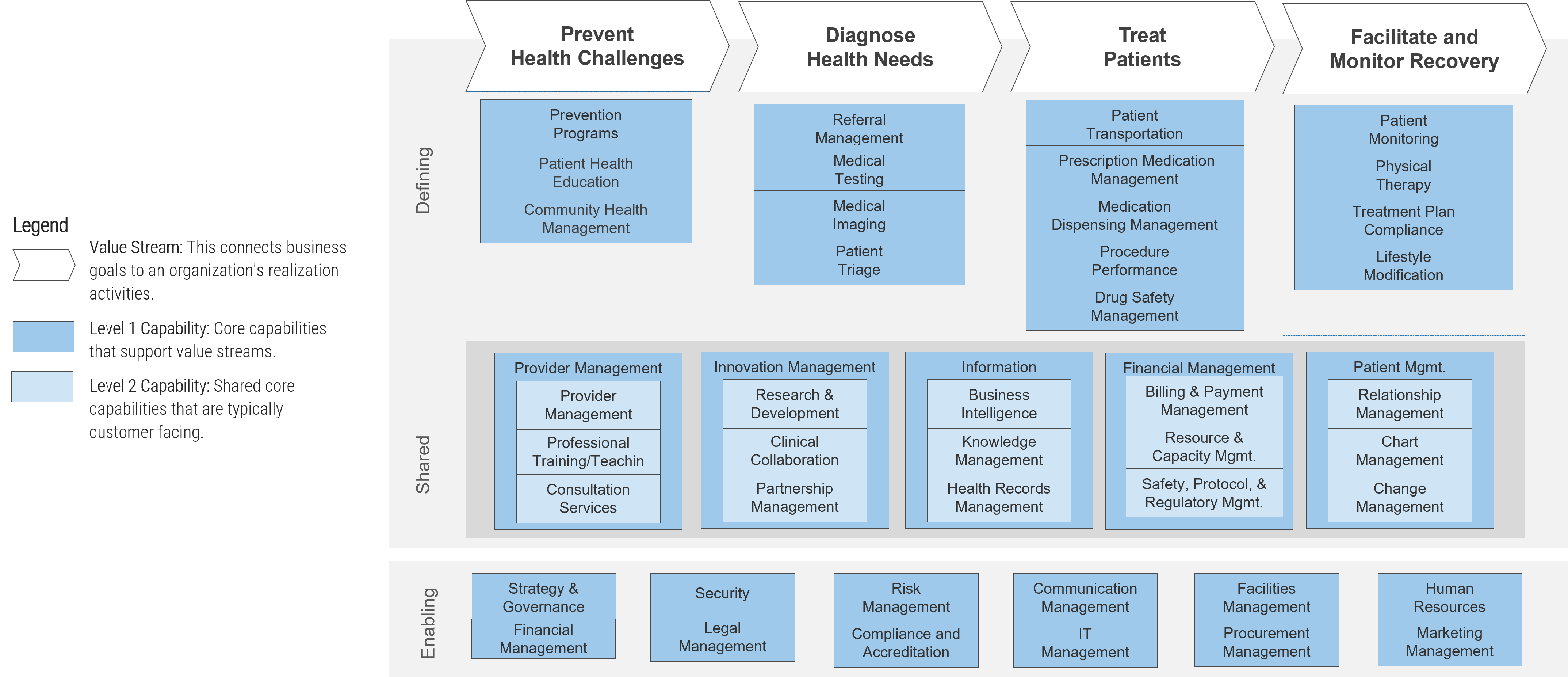
Download Info-Tech’s Industry Reference Architecture for Healthcare
